
The vision that started this company – and continues to drive us – is to create a better experience for the patient. Water vapor is an ideal tool for accomplishing this goal. It is simple, natural, and gentle, but powerful.
Michael Hoey
Founder and Chief Technology Officer
Harnessing the Power of Phase Shift Energy
Prostate tissue ablation by water vapor utilizes the vast amount of energy generated when liquid water changes to water vapor (steam).
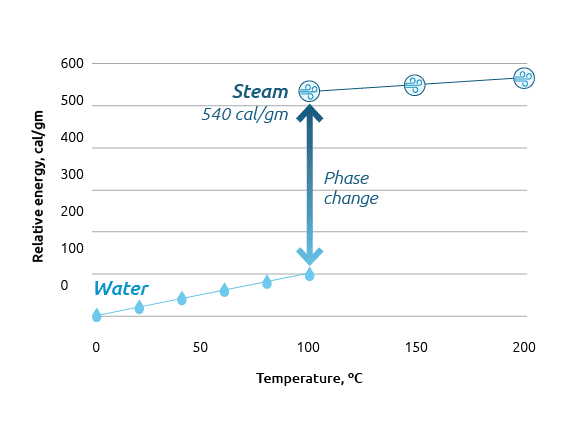
![]() Water Thermal Energy =
Water Thermal Energy =
1 cal/gm/degrees C
![]() Vapor Thermal Energy =
Vapor Thermal Energy =
540 cal/gm @ 100 degrees C
Thermodynamic energy of water vapor
As water converts to vapor (or steam) at ~100°C, an exponential phase shift occurs, with the resulting water vapor carrying more than 5x the energy of water of the same mass.
The Vanquish® System is designed to use the phase shift energy stored in sterile water vapor to transfer thermal energy to targeted prostate tissue, causing cell death.
A New Ablation Energy Modality
Vapor is delivered to the target prostate tissue and, as it reverts to it’s liquid state, stored thermal energy is released directly onto the cell membranes, causing cell destruction.
During a Vanquish procedure, sterile water is converted to vapor and delivered through a needle-shaped catheter with a porous distal tip placed within the targeted tissue. Interstitial fluid-filled spaces surround prostate cells. During multiple treatments, vapor exits the catheter at a higher pressure than the extracellular environment, moving convectively through prostate tissue, displacing interstitial fluid, and reaching cell membranes. Rapid phase transformation of water vapor back to its liquid state (condensation) releases the stored latent heat of vaporization directly onto the affected cell membranes, denaturing them and causing cell death.
A Difference in Time and Transmission
Videos representing the difference between the conductive and convective transfers of thermal engery.
Respecting Natural Boundaries
Unlike traditional ablation technologies, water vapor transfers energy convectively. The natural boundaries of the prostate are effective physical barriers to the movement of vapor.
A distinction between thermal water vapor and other ablative technologies: when vapor is released within one of the prostate zones, it tends to “respect” the boundaries of the prostate capsule and pseudo capsule by staying within the zone it was released.
This feature of vapor is critical when ablating targeted prostate tissue because it prevents the ablative energy in the vapor from escaping outside of the prostate.
Containing the energy within the targeted zone reduces the potential for incidences of erectile dysfunction and urinary incontinence, which are commonly experienced with traditional treatments.
We’re Here
To Help.
Francis Medical would love to connect. Follow us on social media or complete the form to ask a question or be added to our company communications.


 Refer to the device User Manual for a list of contraindications, warnings, and cautions.
Refer to the device User Manual for a list of contraindications, warnings, and cautions. Training: Do not operate the Vanquish System without completing Francis Medical-provided physician training. Untrained operation of the device may lead to improper use. Improper use can result in patient injury or equipment malfunction.
Training: Do not operate the Vanquish System without completing Francis Medical-provided physician training. Untrained operation of the device may lead to improper use. Improper use can result in patient injury or equipment malfunction.